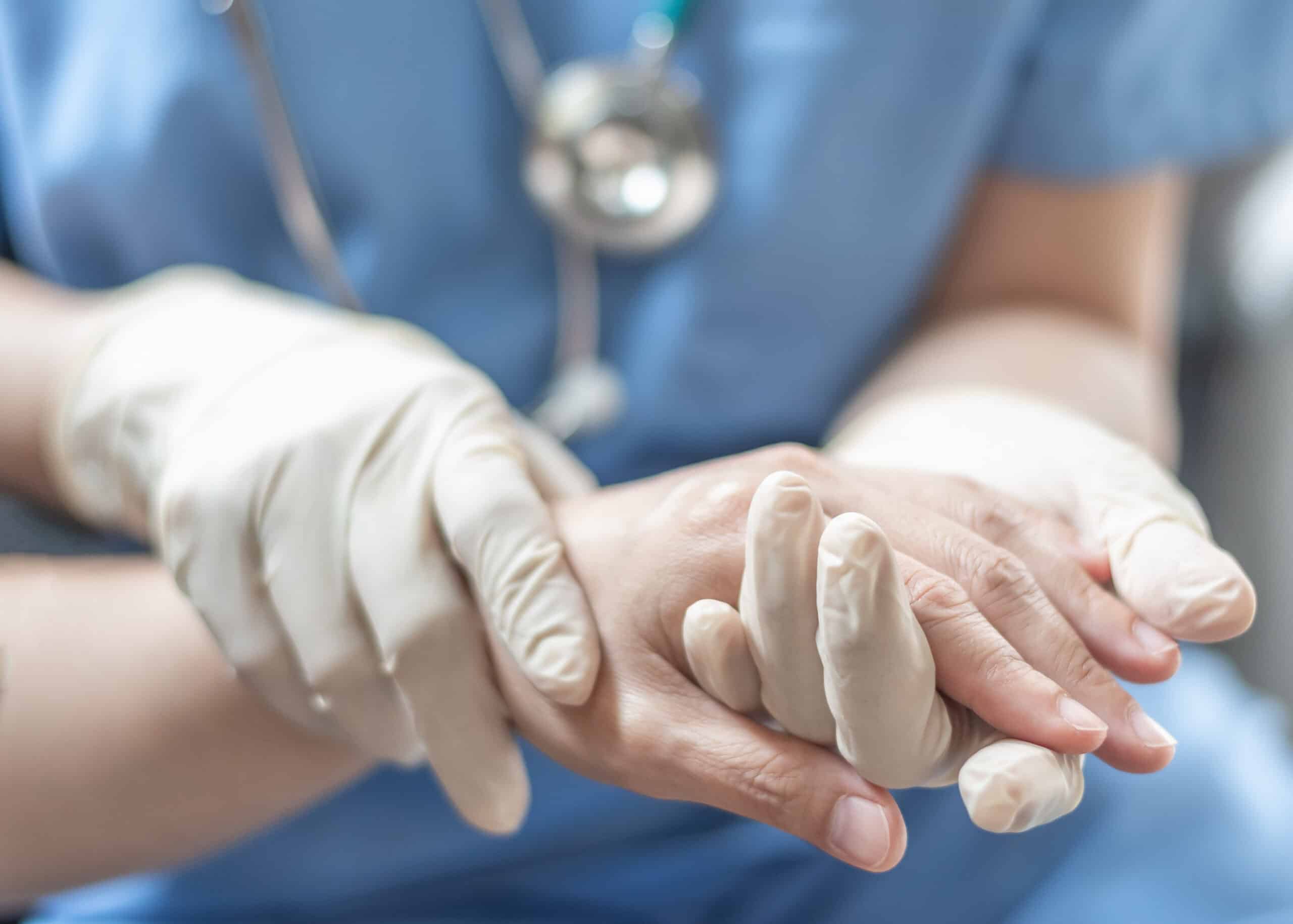
At the Mayo Clinic’s Conference on Brain Health & Dementia, PMC Co-director Jason Karlawish, MD, was a featured speaker. Dr. Karlawish told three stories of significant figures that demonstrate the influence of politics and culture on Alzheimer’s disease research and care.
Archives for 2021
Jason Karlawish’s Recommended Reads
By Jason Karlawish
2021 was a big book year for me.
Yes of course, there was mine. Conversations and correspondence with readers of The Problem of Alzheimer’s were enlightening and inspiring. So too was reading the following.
Three books rounded out my understanding of the experiences of either being a person with disabling and progressive cognitive impairments caused by diseases such as Alzheimer’s disease, or of caring for that person.
Recommended reads from PMC faculty and staff
As the year comes to a close, the faculty and staff of the Penn Memory Center offer you their favorite books they read in 2021. Click the book title to learn more and purchase.
When the Eye on Older Patients Is a Camera
In the middle of a rainy Michigan night, 88-year-old Dian Wurdock walked out the front door of her son’s home in Grand Rapids, barefoot and coatless. Her destination was unknown even to herself.
Wurdock was several years into a dementia diagnosis that turned out to be Alzheimer’s disease. By luck, her son woke up and found her before she stepped too far down the street. As the Alzheimer’s progressed, so did her wandering and with it, her children’s anxiety.
“I was losing it,” said her daughter, Deb Weathers-Jablonski. “I needed to keep her safe, especially at night.”
Video: Diet, Aging, and Your Brain
Patricia St. Ledger, MS, RD, LDN, describes the importance of a brain-healthy diet at any age and provides examples of meals that fit into a variety of lifestyles and diets. Her presentation was part of the Penn Memory Center’s Healthy Aging Series.
PMC, English Department jointly host celebration of John Keats

Nineteenth century romantic poet John Keats was influenced by more than just nature and beauty — he was intimately familiar with disease and medicine.
At the special medical humanities event John Keats: Scientist and Poet hosted by the Kelly Writers House, Penn Memory Center Co-director Jason Karlawish, MD, and Penn English Professor Toni Bowers, PhD, led a conversation exploring the ways in which Keats’ brief medical experience shaped him as a poet.
Why and Where to Get Your COVID-19 and Flu Vaccines this Fall
It has been almost two years since the COVID-19 pandemic impacted us all, and almost six months since we last shared with you the importance of vaccination. We have seen many changes to procedures and daily life — adapting as we learn new information. Like us, viruses also learn ways to adapt. There is an emergence of a new COVID-19 variant called Delta. Viruses change and adapt overtime, acting in new ways. The longer a virus circulates, the more it can change. This is called a variant. As the Delta variant has emerged, we would like to encourage you to get your COVID-19 vaccinations.
Below are some facts about the Delta variant from the Centers for Disease Control:
- The Delta variant is more contagious
- Some data suggest the Delta variant might cause more severe illness than previous variants in unvaccinated people
- Unvaccinated people remain the greatest concern
- Fully vaccinated people with Delta variant breakthrough infections can spread the virus to others. However, vaccinated people appear to spread the virus for a shorter time
- Vaccines in the US are highly effective, including against the Delta variant
Medical student at PCOM, member of Alpha Phi Alpha, and Penn Memory Center community partner Frederick Okoye shared his thought on the COVID-19 vaccination. “It’s just peace of mind. It’s just looking out for your fellow man or woman in your communities. Looking out for our elderly, looking out for our immunocompromised. It’s doing your civil duty.” Okoye said. “If you’re lucky enough to get the vaccine, I strongly encourage anybody to do so.”
Older adults, loved ones respond similarly to Alzheimer’s risk

If a son heard that his father had an increased risk of Alzheimer’s disease, based on a beta-amyloid PET scan, he would likely experience negative emotions such as sadness, worry, disappointment, and concern for his own risk of cognitive decline.
By Varshini Chellapilla and Lindsey Keener
If you were told your spouse’s risk level for developing Alzheimer’s disease, how would you react, knowing you would become their closest caregiver? If you were to be told your sibling’s risk for developing Alzheimer’s disease, how would you react, knowing you share some genetic makeup?
Emily Largent, PhD, JD, RN, member of the Penn Program on Precision Medicine for the Brain (P3MB), studies the implications of test results that can inform an older adult of their risk for Alzheimer’s disease later in life. But, as she explains, more people are affected by an Alzheimer’s disease diagnosis than the patient alone.
And, her research showed, both older adults and their loved ones had similar responses to news of the older adult’s risk.
Jason Karlawish’s new book examines “The Problem of Alzheimer’s: How Science, Culture, and Politics Turned a Rare Disease Into a Crisis and What We Can Do About It” — Dementia in Europe
Dr. Jason Karlawish, co-director of the Penn Memory Center at the University of Pennsylvania in Philadelphia, USA, spoke to Alzheimer Europe about his new book, which takes us inside laboratories, the homes of people living with dementia, carers’ support groups, progressive care communities, and Dr. Karlawish’s own practice at the Penn Memory Center.
PMC, former fellow jointly consider impact of tau-free Alzheimer’s pathology

Dr. Lauren McCollum poses in the Perelman Center for Advanced Medicine during her time at Penn Memory Center. (Credit: Terrence Casey)
By Lindsey Keener
It’s been more than a year since Lauren McCollum, MD, concluded her time as a trainee at Penn Memory Center, but mentorship and grant support have kept her in close collaboration with the site of her fellowship.
While at Penn, Dr. McCollum was a medical student at the Perelman School of Medicine, a neurology resident, and ultimately a Cognitive and Behavioral Neurology Clinical Fellow at PMC. Today she is a clinician and researcher at the University of Tennessee’s Pat Summitt Clinic. She is also a clinical assistant professor at the university.
At both centers, her ultimate priority was the same: to give quality care to each of her patients and their families.
“There’s this amazing human component to this where you’re supporting families and supporting people going through something that is really, really hard,” she said. “A slow, chronic, often fatal progressive disease of the brain.”
A Celebration of Hope: Training
Training programs to advance care, research, and equity
The Penn Memory Center offers valuable hands-on experience and mentorship through training programs in the areas of social work, research, neuropsychology, communications, and clinical care and is dedicated to creating training opportunities for people from underrepresented racial and ethnic groups. These efforts play a vital role in advancing Alzheimer’s disease and related dementias (ADRDs) care and research and closing health disparity gaps. Funding of our training programs relies on generous donations.
A Celebration of Hope: Clinical Care
Quality Care Matters
The Penn Memory Center’s expert team of health professionals is dedicated to providing the highest standard of clinical care to patients. This quality care is difficult to find elsewhere in Philadelphia, and the number of PMC patients is increasing. We need your support to continue serving our growing patient community.
A Celebration of Hope: Programming
PMC programming: inclusive, engaging, and free-to-all
From our classic, evidence-based programs such as Caregiver Educational class and Memory Cafe to newer, trailblazing programs like Mindfulness & Meditation Class, Cognitive Comedy, and Healthy Aging Series, PMC is always growing and evolving to best serve its families and build community. These important programs rely on philanthropic support to keep them running and free-to-all.
A Celebration of Hope: Research
Research is made possible by you
Research moves us closer to a treatment and to a better future for patients and their loved ones. At PMC, we conduct a variety of research — from clinical trials testing novel drugs to studies about patient and caregiver experiences. Our dedicated participants and funding make this research possible.
A Celebration of Hope: Community Outreach
Community outreach promotes health equity
In collaboration with our community partners, PMC provides health education, services, research, and job opportunities to the West Philadelphia community in effort to create more equitable health outcomes. This work relies on the funding of our generous supporters.
Kicking-off “A Celebration of Hope”
Oct. 3 marks the start of the Penn Memory Center’s annual fundraiser, A Celebration of Hope! This is an asynchronous virtual event that features an online auction. The auction will open for bidding on Oct. 5 at 12 p.m. and close on Oct. 8 at 12 p.m. Click here to register for our auction.
A Celebration of Hope welcome video
Thank you and farewell to Sharon Best

“Sharon is an exceptional practitioner and colleague,” said PMC Executive Director Felicia Greenfield, MSW, LCSW. “She consistently goes above and beyond to care for our patients and their families.”
Best’s primary duty was assisting the team of neurologists, geriatricians, social workers, and neuropsychologists in developing innovative approaches to the diagnosis and treatment of Alzheimer’s disease.
“A curious professional, Sharon delighted in challenging herself to learn new things and she enthusiastically shared her knowledge with others,” said Greenfield.
Virtual programming at the Penn Memory Center — Fall 2021
Cognitive Comedy • Tuesdays 1:30 – 3:00 p.m.
Cognitive Comedy is a free improv comedy workshop for people with cognitive impairment and their loved ones. Participants can get out of their own heads and experience “group mind” while learning about improv comedy. This program starts on September 21. Register for Cognitive Comedy.
Dr. Jason Karlawish to be featured speaker at inaugural Mayo Clinic Conference on Brain Health and Dementia
Penn Memory Center Co-director Jason Karlawish, MD, will be the featured speaker at the Mayo Clinic’s first Conference on Brain Health and Dementia. The Conference will take place October 29 from 10:15 a.m. to 4:00 p.m. EST. The Conference will recognize all that people who live with dementia and their families have experienced during the COVID-19 pandemic, and experts will cover the latest on brain health and dementia research.
Seeking Early Signals of Dementia in Driving and Credit Scores — The New York Times
Dr. Jason Karlawish and Dr. Emily Largent offer their takes on using driving performance and credit scores to predict the onset of dementia. Should entities like auto insurance companies have access to test results of these predictors? Dr. Largent weighs in.
Farewell to Melissa Johnston Esparza, clinical research coordinator
By Cait Kearney

“PMC is a wonderful organization, and having been a part of helping advance its mission has been a rewarding experience I will cherish forever,” Johnston Esparza said.
Johnston Esparza joined PMC as a clinical research coordinator for the REVEAL-SCAN Study (Risk Evaluation and Education of Alzheimer’s Disease: The Study of Communicating Amyloid Neuroimaging), a project investigating the impact of learning one’s personal risk of having Alzheimer’s disease on thinking and health behaviors.
“Melissa is a stellar coordinator. She stepped into a study that was in distress and quickly turned it around and into a great scientific success,” said Jason Karlawish, MD, co-director of PMC and co-principal investigator of the REVEAL-SCAN Study.
Recently Approved Alzheimer Drug Raises Questions That Might Never Be Answered — JAMA Network
In JAMA Network Medical News, Dr. Jason Karlawish expressed his concern that Aduhelm’s approval will have a negative impact on the enrollment of future clinical trials.
Thank you, Matt!

Matthew Ferrara, MS Ed., is leaving the Penn Memory Center (PMC) after three years as a clinical research coordinator.
“Matt has been an absolute delight to work with in his time here at the PMC,” said PMC Co-Director David Wolk, MD, “Matt will be missed by our faculty, staff, and research participants.”
Ferrara joined PMC in 2018 as a coordinator for PMC’s largest study — the Aging Brain Cohort (ABC) Study. Data collected through the ABC Study is used by scientists across the nation and the world to research Alzheimer’s disease and life-long brain health.
“He displayed a remarkable dedication to the success of the ABC study to the benefit of our research participants and the numerous studies that depend on these data,” Dr. Wolk said.
The harrowing new reality for Alzheimer’s patients — Vox
In a recent Vox article, assistant director of social work Alison Lynn, MSW, PMC researcher Emily Largent, PhD, JD, RN, and PMC co-director Jason Karlwish, MD, offered insight into the uncertainties people with an Alzheimer’s disease diagnosis and their caregivers may face and discussed the added stress they may feel from the controversy around Aduhelm. (Image: Christina Animashaun/Vox)
In Reversal, F.D.A. Calls for Limits on Who Gets Alzheimer’s Drug — The New York Times
The Food and Drug Administration (FDA) has revised its recommendation of who should receive Aduhelm, the controversial Alzheimer’s disease drug approved by the FDA last month.
The original label stated the treatment was for anyone with Alzheimer’s disease, encompassing six million Americans. Under the new label, the FDA recommends Aduhelm to “patients with mild cognitive impairment or mild dementia stage of disease,” reflecting the population tested in clinical trials and cutting the number of eligible Americans to about two million.
“The revision of this label is yet another piece of evidence that should cause the American public to be concerned about how FDA is practicing its regulatory science,” PMC co-director Dr. Jason Karlawish told the New York Times.
Thank you, Hannah!
By Varshini Chellapilla
Cao was a candidate for the master of social work at the University of Pennsylvania School of Social Policy & Practice when she joined P3MB researcher and clinical psychologist Shana Stites, PsyD, MA, MS, on the Gender’s Impact on Cognition in Older Adults (CoGenT3) study.
“Hannah is amazing,” Dr. Stites said. “She showed up uncertain about research, then took to it like a fish to water. She quickly became the cornerstone of the COGENT3 study and has been a pleasure to mentor. She’s going to continue to do great at all she does.”
The controversial approval of an Alzheimer’s drug reignites the battle over the underlying cause of the disease — The Washington Post
Dr. Jason Karlawish, co-director of PMC, was quoted by The Washington Post regarding the negative potential consequences of the Food and Drug Administration’s approval of Aduhelm.
“Companies are companies, I can’t fault them for doing what companies do, but we have now unleashed drugs that we are not sure what the benefits are, and that could have enormous consequences,” said Dr. Jason Karlawish.
A New Alzheimer’s Drug Offers More Questions than Answers — The New York Times
PMC co-director Dr. Jason Karlawish was quoted in The New York Times regarding the uncertainties surrounding Aduhelm, the Alzheimer’s disease drug recently approved by the Food and Drug Administration. When asked if adults should consider Aduhelm, Dr. Karlawish said, “The F.D.A. has passed the determination along to the American family.”
6 children’s books about Alzheimer’s disease and dementia
Understanding the way that Alzheimer’s disease and related dementias affect loved ones is a hard concept for many adults to wrap their head around. For children, it might seem tougher to explain and comprehend.
Alison Lynn, MSW, LCSW, associate director for social work at the Penn Memory Center, suggests children’s books as a way to introduce a diagnosis to them and its effects on their relationships with older loved ones.
“We get a fair number of questions regarding grandchildren in families that live together intergenerationally,” Lynn said. “Questions are more commonly focused on what to do after the diagnosis and the real-world issues that arise than about how to explain the diagnosis itself. Situations like these have also increased due to the pandemic.”
Children’s books that address dementia and Alzheimer’s disease help relay the concepts that are less concrete and harder to grasp.
Introducing the 2021-2022 PMC Clark Scholars
By Varshini Chellapilla
At the Penn Memory Center and the Alzheimer’ Disease Research Center at the University of Pennsylvania, we are committed to training the next generation of clinicians and researchers. The Christopher M. Clark Scholars program was created to encourage and guide early career researchers as they study the various aspects of Alzheimer’s disease, mild cognitive impairment, cognitive aging, and lifelong brain health.
This year’s scholars are Lasya Sreepada, Xueying Lyu, Brianna Morgan, Kyra O’Brien, and Nicole Nissim, who come from diverse backgrounds in bioengineering, nursing and clinical research.
Christopher M. Clark was the founding director of the Penn Memory Center. Among his many accomplishments were his role in the team that demonstrated the ability of a florbetapir PET scan to detect brain deposits of beta-amyloid, his co-development of the Dementia Severity Rating Scale, and contributions to the development of therapies for Alzheimer’s disease.
The scholars program at PMC was renamed last year to be the Christopher M. Clark Scholars Program to honor Dr. Clark’s achievements as well as his dedication to research and promoting awareness of Alzheimer’s disease.
PMC Community Discussion on Aduhelm (aducanumab)
This past Wednesday, the Penn Memory Center held a community event for PMC patients and families led by co-directors Drs. Jason Karlawish and David Wolk to discuss the Food and Drug Administration’s (FDA) decision to approve Aduhelm (aducanumab). The focus was the impact of the approval on the PMC’s clinical and research operations.
Alzheimer’s Doctors On Biogen’s New Drug; Tax Inequality — NPR Here & Now
Decision to Approve New Treatment for Alzheimer’s Disease – FDA
By Dr. Patrizia Cavazzoni, Director, FDA Center for Drug Evaluation and Research
Today FDA approved Aduhelm (aducanumab) to treat patients with Alzheimer’s disease using the Accelerated Approval pathway, under which the FDA approves a drug for a serious or life-threatening illness that may provide meaningful therapeutic benefit over existing treatments when the drug is shown to have an effect on a surrogate endpoint that is reasonably likely to predict a clinical benefit to patients and there remains some uncertainty about the drug’s clinical benefit.
This approval is significant in many ways. Aduhelm is the first novel therapy approved for Alzheimer’s disease since 2003. Perhaps more significantly, Aduhelm is the first treatment directed at the underlying pathophysiology of Alzheimer’s disease, the presence of amyloid beta plaques in the brain. The clinical trials for Aduhelm were the first to show that a reduction in these plaques—a hallmark finding in the brain of patients with Alzheimer’s—is expected to lead to a reduction in the clinical decline of this devastating form of dementia.
We are well-aware of the attention surrounding this approval. We understand that Aduhelm has garnered the attention of the press, the Alzheimer’s patient community, our elected officials, and other interested stakeholders. With a treatment for a serious, life-threatening disease in the balance, it makes sense that so many people were following the outcome of this review. Further, the data included in the applicant’s submission were highly complex and left residual uncertainties regarding clinical benefit. There has been considerable public debate on whether Aduhelm should be approved. As is often the case when it comes to interpreting scientific data, the expert community has offered differing perspectives.
At the end of the day, we followed our usual course of action when making regulatory decisions in situations where the data are not straightforward. We examined the clinical trial findings with a fine-tooth comb, we solicited input from the Peripheral and Central Nervous System Drugs Advisory Committee, we listened to the perspectives of the patient community, and we reviewed all relevant data. We ultimately decided to use the Accelerated Approval pathway—a pathway intended to provide earlier access to potentially valuable therapies for patients with serious diseases where there is an unmet need, and where there is an expectation of clinical benefit despite some residual uncertainty regarding that benefit. In determining that the application met the requirements for Accelerated Approval, the Agency concluded that the benefits of Aduhelm for patients with Alzheimer’s disease outweighed the risks of the therapy.
Click the headline or the button below to read this announcement on the FDA website.
If the FDA approves Biogen’s Alzheimer’s treatment, I won’t prescribe it — STAT News
In a recent essay published in STAT News, PMC co-director Dr. Jason Karlawish argued that, given aducanumab’s “incomplete and contradictory” data and the results of an analysis of aducanumab’s effectiveness and value by the Institute for Clinical and Economic Review, the FDA should not approve the drug at this time and stated he will not prescribe it to his patients.
Click the headline or the button below to read this article on STAT News.
Neurology Training Steps Up to Focus on Racism and Social Injustice — Neurology Today

Roy H. Hamilton, MD, MS, FAAN, associate professor of neurology and assistant dean for cultural affairs and diversity at University of Pennsylvania’s Perelman School of Medicine, said neurology training would be lacking without an emphasis on racial disparities, especially since many neurologic conditions are more prevalent in minority communities. The neurology department at UPenn began to focus on diversity and inclusion in its training program in 2017, but the initiative is now seen as the core of everything the department does, from hiring to promoting staff to training students and residents.
Dr. Hamilton sees patients in the Penn Memory Center clinic.
Click the headline or the button below to read this article on Neurology Today.
Penn Just Launched a Neurological Clinic for COVID-19 Long Haulers — Philadelphia Magazine

Click the headline or the button below to read this article on PhillyMag.com.
Detecting and treating Alzheimer’s before symptoms set in, with Dr. Jason Karlawish — BeingPatient.com
As part of its LiveTalk series, Being Patient spoke with Dr. Jason Karlawish, co-director of the Penn Memory Center and author of “The Problem of Alzheimer’s,” about the advances in dementia research and diagnostics that have allowed for the early detection of Alzheimer’s. Click the headline or the button below to read this article on BeingPatient.com.
‘That would be dreadful’: Researchers study thought process behind revealing Alzheimer’s test results

By Varshini Chellapilla
If you tested positive for a biomarker of Alzheimer’s disease, whom would you tell? Why?
Penn Program on Precision Medicine for the Brain (P3MB) researcher Emily Largent, PhD, JD, RN, conducted two qualitative studies to understand individuals’ decision-making process as they choose whom, why and how to share information regarding their Alzheimer’s disease biomarker and genetic testing results. The study, titled “‘That would be dreadful’: The ethical, legal, and social challenges of sharing your Alzheimer’s disease biomarker and genetic testing results with others,” was published in the Journal of Law and the Biosciences on May 19.
The studies were done in collaboration with three other researchers from Penn Program on Precision Medicine for the Brain (P3MB): Shana Stites, PsyD, MS, MA; Kristin Harkins, MPH; and Jason Karlawish, MD.
Thank You, Grace!
By Varshini Chellapilla
Clinical Research Project Manager Grace Stockbower, MPH, is moving on from the Penn Memory Center after eight years.
Stockbower came to the center as a research specialist in 2013, after studying psychology and neuroscience at Haverford College. She worked exclusively on studies led by Dave Wolk, MD, PMC co-director.
“We are extremely lucky that we had an opportunity to work with Grace over these last 8 years,” said Dr. Wolk. “She has played a tremendous role in the culture and operation of the Penn Memory Center and our research studies.
Penn researchers study patterns of atrophy in the brain using high-field MRIs
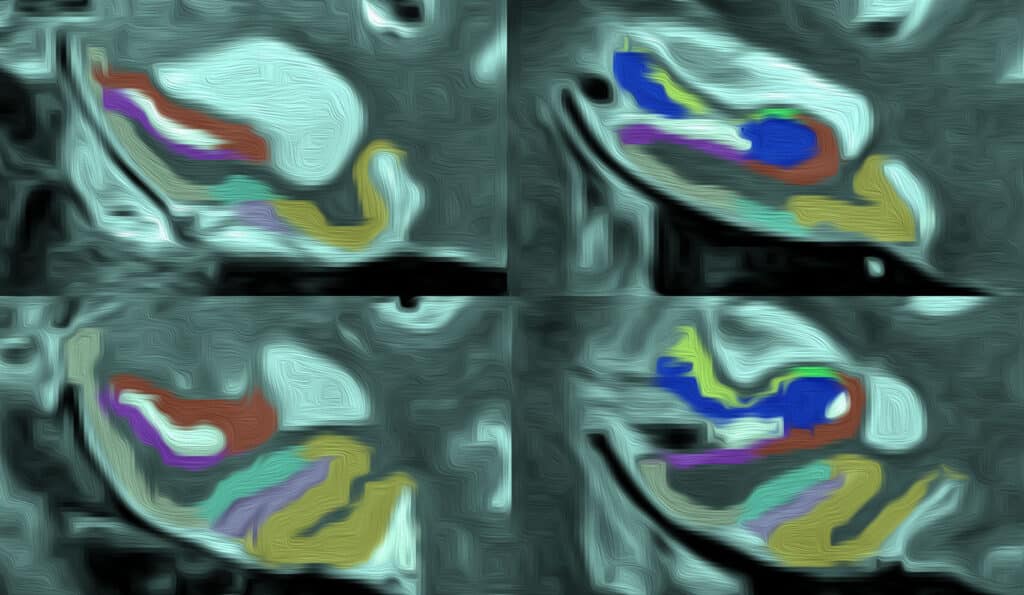
Graphic illustration of a T2-weighted MRI with MTL subregion segmentation.
By Varshini Chellapilla
Specialized high-field MRI scanners are some of the most advanced machines in medical research currently and have been equipped to study epilepsy, neurological disorders, and Alzheimer’s disease across many research fields. At Penn, the ultra-high-definition resolution of these MRIs helped researchers study the patterns of atrophy, or loss in volume due to degeneration of cells, in patients with semantic variant primary progressive aphasia (svPPA).
“Volume loss in this region of the brain has been investigated in the past but never with scans as good as these,” said Laura Wisse, PhD, the principal investigator for the study. “With higher resolutions, we were able to measure this particular region of the brain in a much more detailed way.”
NIA publishes book on exercising for older adults
By Varshini Chellapilla
Exercise is a key component of maintaining healthy cognitive abilities among older adults. Many studies have shown that physical activity and fitness can lead to improvements in memory retention as well as a reduced risk for cognitive decline.
The National Institute on Aging (NIA) published an exercise book focused on the methods and benefits of physical exercise for older adults. Titled “Get Fit For Life: Exercise & Physical Activity for Healthy Aging,” the book is available to order or download for free on the NIA website.
The book is designed for beginners as well as regular exercisers and provides detailed instructions for simple exercises, worksheets to help construct fitness routines, and activity logs. Also included is a special section designated for older adults with chronic conditions such as arthritis, Alzheimer’s disease, and type 2 diabetes. From stretches between TV commercials to yoga routines, the book comes with links to organizations such as the YMCA who have designed exercise programs that build on endurance, mobility, balance, and strength.
PMC researchers receive $3.5M grant, launch ABCD2 study to address disparities in Alzheimer’s research

Black adults are underrepresented in Alzheimer’s disease research, even though they are more likely to develop the disease. The Aging Brain Cohort Study Dedicated to Diversity will seek to enroll more Black participants like Jay Austin (above), to combat this disparity. Austin cited this disparity as his motivation for participating in research.
Black adults are more likely than other groups to develop Alzheimer’s disease or related disorders but are poorly represented in Alzheimer’s disease research, including recent clinical trials. This health disparity illustrates how Black individuals can benefit from advances in the field if they had access.
This week, the Pennsylvania Department of Health’s Commonwealth Universal Research Enhancement (CURE) program announced it will award a $3.5 million grant to Penn Memory Center (PMC) researchers and community partners to address the underrepresentation of Black adults in Alzheimer’s disease research. The grant supports the Aging Brain Cohort Dedicated to Diversity (ABCD2) study, a research and training initiative led by David Wolk, MD, a professor of Neurology in the Perelman School of Medicine at the University of Pennsylvania. Wolk is also the incoming director of the Alzheimer’s Disease Research Center, and PMC co-director.
PMC Partner: Getting COVID vaccine ‘really about this community’

By Sharnita Midgett
On Feb. 24, Penny Scott-Sedley walked into the Perelman Center, eager for her chance to move towards a safer world after a year of the pandemic.
As an ABC participant, normally she would hear from Penn Medicine about her upcoming ABC visit. However, this time, she received an email from Penn Medicine informing her that she could schedule her appointment for the first dose of the COVID vaccine. Scott-Sedley knew that there would be spring-like weather in Philadelphia on Feb. 24, so with excitement, she planned to receive her dose that Wednesday.
“I always was eager to become vaccinated once a vaccine was developed. It didn’t occur to me not to, especially not after it was reported that Blacks in this country were experiencing a much higher incidence of serious illness once contracting the virus and succumbing to it in higher numbers,” Scott-Sedley began.
Her appointment time was busy, but she noted that the process was extremely well-organized.
“It took no time to get through to the person who would perform the jab, and the wait afterwards for monitoring any adverse reactions was easy-peasy.”
She had no reactions after receiving the first dose of the Pfizer vaccine.
“As a Black woman of a certain age, I was aware of the historical struggle that Blacks have faced from racist and unethical scientists. Think the horrific Tuskegee Institute Scandal. But in this instance, we would not be singled out for the vaccine to the exclusion of other groups. So I considered it to be a safe bet.”
Caregiver Forums offer solidarity, solace in virtual meetings
By Varshini Chellapilla
Six out of seven days a week, Deborah Maser used to drive herself to Trenton, New Jersey to a jazzercise class in the mornings. She was diagnosed with mild cognitive impairment in 2018 and was an avid jazzerciser. On Wednesdays, her husband used to take the train to Philadelphia to teach at the University of Pennsylvania School of Dental Medicine. Her daughters would visit her that day to make sure she wasn’t alone for more than a few hours.
A routine had been set, only to be disrupted in March.
“When the pandemic struck, jazzercise had stopped – as did dental school, of course – for several months,” Dr. Maser said. “And it became a little bit more stressful because my wife had nothing to do in the mornings.”
The pandemic has seeped into nearly every aspect of caregivers’ lives. With increased health risks, mental stress and adjustments to a virtual world, caregivers across the country found themselves faced with new challenges.
The Penn Memory Center (PMC) began the Caregiver Forums in March 2020 in an attempt to provide caregivers a space where they could talk freely and share advice as they learned to navigate caring for their loved ones during the pandemic.
Pragmatic trials — when good research means no informed consent

Most research is conducted with informed consent, a process that allows to the prospective participant to learn about the study through discussion with the investigator or study staff and to decide if participating is right for them. Yet, there are exceptions. In limited and strict circumstances, federal regulations governing human subjects allow for alterations or even waivers of informed consent. (Adobe Stock)
by Varshini Chellapilla
Most clinical trials are conducted in highly controlled environments to study the efficacy of a certain intervention. But the world we live in is often much messier than that.
This is where pragmatic trials come in. Pragmatic trials are designed to study interventions in circumstances that closely approximate actual clinical practice as closely as possible. Some pragmatic trials include subjects who may not know that they are part of a clinical research.
Research conducted by Penn Program on Precision Medicine for the Brain Researcher Emily Largent, PhD, JD, RN, and Stephanie Morain, PhD, MPH, an assistant professor at the Center for Medical Ethics and Health Policy at Baylor College of Medicine, looked at the data on public attitudes toward consent for pragmatic trials. The resulting article, published in The Hastings Center Report on April 11, was titled “Public Attitudes toward Consent When Research Is Integrated into Care—Any ‘Ought’ from All the ‘Is’?”
“In order to make research as much like normal life or regular clinical practice as possible, it is often the case that we want to conduct the research without getting informed consent from participants,” Dr. Largent said. “Because once we tell people they’re in research, that can change what happens and who participates.”
Launching the chronicle of a disease of autonomy: PMC hosts book release event for Jason Karlawish’s ‘The Problem of Alzheimer’s’
By Varshini Chellapilla
“Imagine a healthcare system incapable of diagnosing whether increasing numbers of older adults with weight loss, vague pains and anemia have cancer and, if they did, incapable of treating their cancer and caring for their common complications, such as pain and fatigue. That’s the problem for funding older adults with memory loss. The system is broken and a correction is needed to remedy this.”
An excerpt from Penn Memory Center (PMC) Co-Director Jason Karlawish’s new book “The Problem of Alzheimer’s: How Science, Culture and Politics Turned a Rare Disease Into a Crisis and What We Can Do About It,” the paragraph summarizes the roadblocks faced by people with Alzheimer’s disease and caregivers as they navigate the healthcare system, as identified by Dr. Karlawish.
On March 18, Dr. Karlawish read an excerpt from his book and answered questions about the revolutionary moments of Alzheimer’s disease history, the names of experimental Alzheimer’s drugs, and his personal evolution as a physician at a virtual launch event hosted by PMC to commemorate the release of the book.
Dr. Shana Stites named assistant professor of psychiatry

Shana Stites, PsyD, MA, MS, was named assistant professor in the Department of Psychiatry at the Perelman School of Medicine.
“I’m so excited for this new adventure. The scientific and professional opportunities are thrilling, and the company couldn’t be better,” said Dr. Stites. “It’s a privilege to have the chance to help improve care and quality of life for persons with Alzheimer’s.”
Penn researchers find no link between anesthesia, dementia
By Varshini Chellapilla
A common question asked of physicians and surgeons is whether anesthesia, generally given during surgeries, is associated with a risk of developing Alzheimer’s disease or other related dementias (ADRD) in the future.
“It’s not an unreasonable notion that anesthesia would affect brain health,” Dr. Wolk said. “Anesthesia has many effects on the brain, and surgery itself is associated with all sorts of systemic changes in the body and brain.”
A new study conducted by Penn Memory Center Co-Director and Alzheimer’s Disease Research Center Director David Wolk, MD, in collaboration with colleagues in the Perelman School of Medicine and The Wharton School, observed elderly patients who were exposed to anesthesia during an appendectomy, a surgical procedure performed to remove the appendix, and then followed post-operation to determine if there was an association between anesthesia and development of clinical Alzheimer’s disease. The study, titled “Alzheimer’s Dementia After Exposure to Anesthesia and Surgery in the Elderly,” was published in the Annals of Surgery in the November 2020 issue.
GCBH: Protecting your brain, mental well-being from COVID-19
PMC co-director Jason Karlawish, MD, coauthored the Global Council on Brain Health’s (GCBH) recent report COVID-19 and Brain Health: The Global Council on Brain Health’s Recommendations on What to Do Now.
Dr. Karlawish is a member of the GCBH and serves on its Governance Committee. The GCBH is an AARP collaborative of scientists, health professionals, scholars, and policy experts from around the world who are working in areas of brain health related to human cognition and who strive to provide the best and most recent scientific insights into brain health to help people lead their best lives.
In their special report, Dr. Karlawish and his fellow GCBH members warn that, in addition to COVID-19’s widely known respiratory effects, the virus can also damage brain health. The report offers ten suggestions to maintain brain health during the pandemic, as well.
PMC researchers look at the future of Alzheimer’s detection
by Varshini Chellapilla
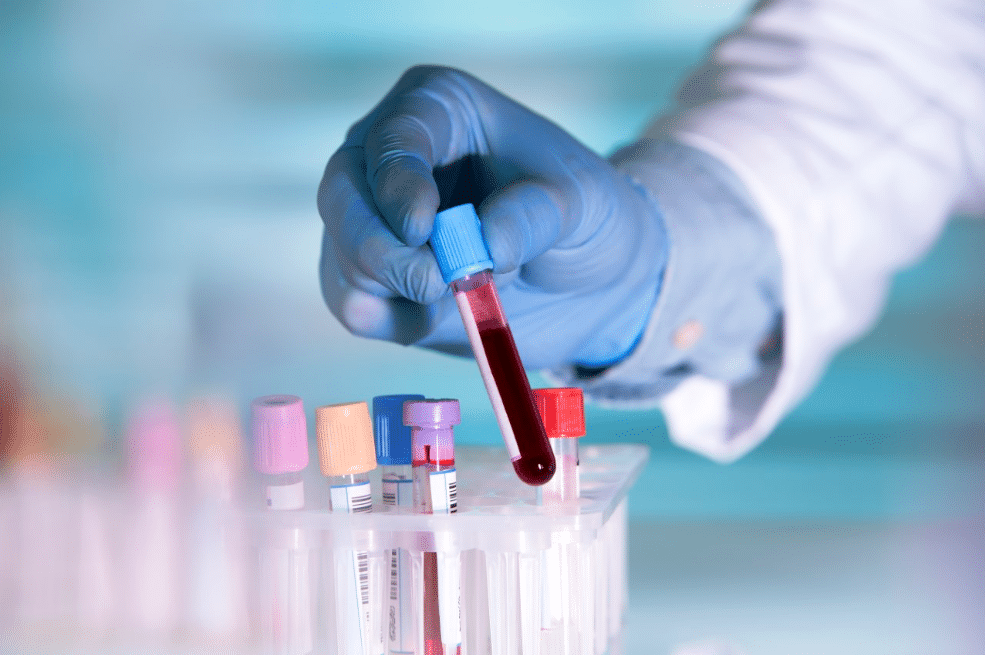
A direct-to-consumer blood test for a key Alzheimer’s biomarker may be “inevitable,” but Penn Program on Precision Medicine for the Brain (P3MB) researchers warn that receiving results from such a test comes with potential challenges.
Penn Memory Center (PMC) Co-Director Jason Karlawish, MD, and P3MB researcher Emily Largent, JD, PhD, RN, with co-author Anna Wexler, PhD, weighed the risks and benefits of these blood tests in a recent article for JAMA Neurology, titled “The Future is p-Tau – Anticipating Direct-to-Consumer Alzheimer’s Disease Blood Tests.”
Alzheimer’s disease has three main biomarkers, or medical indicators in the body that characterize the disease: the build-up of amyloid proteins in the brain disrupting the functions of neurons, the loss of function and structure of neurons, and tau-protein tangles formed inside neurons.
“While amyloid has historically attracted a lot of attention, in the last year, a lot of interest started to grow around blood-based biomarkers, particularly the marker of tau,” Dr. Largent said.